Nurses were among the trained healthcare providers ready for deployment as Hurricane Dorian, a Category 5 storm, pummeled parts of the Bahamas with 185 mph winds and threatened Florida's East Coast.
Teams of nurses and other healthcare providers have been part of the nation's disaster response effort for many of the hurricanes that have devastated areas with high winds and flood waters.
Kathi Harvey, DNP, FNP-BC, NHDP-BC, APRN, a certified National Healthcare Disaster Professional, is one of those nurses trained to deploy as part of the U.S. Disaster Medical Assistance Team. Harvey, an adjunct faculty member at Florida Atlantic University's Christine E. Lynn College of Nursing, in Boca Raton, Fla., spent a month in Puerto Rico after Hurricane Maria, a strong Category 4 storm.
She tells us that while being a member of one of many organizations that provides healthcare relief after disasters is gratifying, there's a lot more to disaster nursing than nurses might realize.
"There's nothing haphazard about an emergency response for storms like Dorian," she said. "Teams are in place and ready to act. Everyone on the team has been trained and prepared to provide care in some of the worst imaginable situations."
Federal government responses by teams such as the Disaster Medical Assistance Team are activated at the time of national incidents after states have asked for the help. The response to any disaster always starts at the local, city or county level and — depending on perceived need — works up to state and federal government intervention, according to Harvey.
"We respond to areas where they've asked for help, where the infrastructure has been overwhelmed, the medical system has been overwhelmed or if the medical facility has been destroyed," she said. "We carry mobile hospitals with us. We put them up and they function as a hospital emergency room. They function as surgical suites. We can do just about anything in them."
What nurses and other healthcare professionals often don't realize is that by the time a hurricane or other disaster happens, it's too late to volunteer for deployment to aid in disaster nursing, according to Harvey.
"Once a disaster is out there and we're watching it, it's already too late for nurses to become involved in these agencies because they have to be vetted," she said. "They have to have background checks. Their licenses have to be checked."
Disaster nursing starts long before the disaster occurs
While Harvey wasn't deployed during Dorian, she was with one of the first teams on the ground in Puerto Rico in 2017. The goal, she said, is not to become part of the problem. Well-meaning people want to help after disasters not realizing the scope of issues. And instead of helping, they might get sick or injured and have to be rescued.
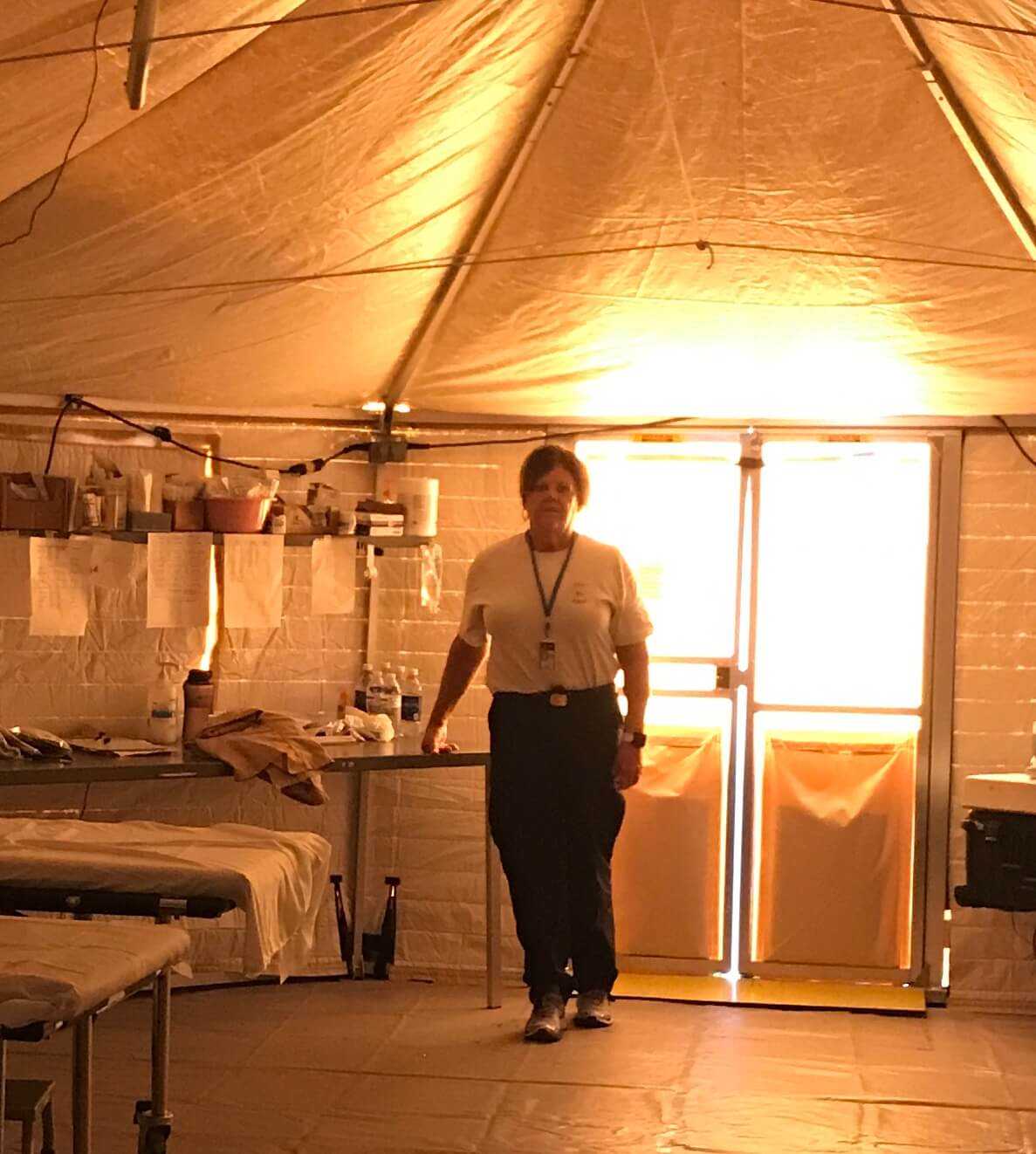
Harvey describes her situation in Puerto Rico as austere. There was no food and water. All she had was the food and water she could carry on her back, according to Harvey.
"The main thrust as in any disaster is food, water, shelter and evacuation," she said. "We have to go back to the lowest level of Maslow's Hierarchy and think, 'What do these people need?'"
People sent clothes after Hurricane Maria to help people in Puerto Rico, but it was extremely hot and there was no way to transport the clothes to the communities. What they needed was food and water, according to Harvey.
"In Dorian's situation, there were already teams on the ground doing pre-planning," she said. "We know from our training that the ports become blocked, the runways will be damaged, so we're going to need shorter range planes or helicopters. We have bases all over the world. In this case, the Coast Guard was prepositioned. They are the best equipped of all the agencies to go in and do search-and-rescue and evacuation, as well as medical care."
Nurses are needed on response teams, according to Harvey. Those who want to get involved in disaster nursing should sign up with an agency, be vetted and go through training long before a disaster hits.
They need to be healthy and fit because nothing is simple in a disaster situation. One example is evacuating a patient from a hospital.
"There are extremely unsafe situations in just getting that patient from the hospital to the helicopter," Harvey said. "[You have to know] how to approach a helicopter. How to keep the patient safe. Once we set the helicopter down, it takes a long time to get it revved up again, so they leave it running with the blades running. There are all kinds of safety procedures that you have to be trained in."
"The other thing that people don't understand is that we are guests in their countries," she said. "This is not part of the U.S. You can't just run in and take people and put them on a plane back to your country. That's illegal."
Other ways to get involved in disaster nursing
Nurses can get involved in disaster nursing response teams in their own communities, according to Harvey.
"There's an organization called the Medical Reserve Corps in which every nurse can get involved," she said.
The corps trains nurses in disaster preparedness, immunization and more. They learn how the National Stockpile works, about local emergency response systems and more.
"That's one way to get extensive training," Harvey said. "The other way is to be active in their hospitals. Each hospital has its own emergency operations command center. At the time of a disaster, it'll be activated and all department heads, pharmacy, nursing, etc., are in one room making decisions about what they're going to do for that disaster."
Should you stay or should you go?
Hospital emergency operations command centers make decisions, including whether to evacuate or shelter in place. Nurses have a lot of input in disaster nursing situations.
For example, nurses need to be aware of what they might need for their patients should the hospital decide to shelter in place. There were hospital, nursing home and assisted-living facility evacuations during Dorian in September. Evacuations usually occur if a hospital or other facility is in harm's way and involve transporting patients to other facilities.
In some cases, only the most fragile patients might be evacuated to another facility, according to Harvey. Hospitals often cancel elective surgeries and discharge all the patients they can before a storm hits.
Nurses are often patient advocates if a patient cannot be discharged because that patient doesn't have anywhere safe to go and wouldn't be a candidate for a shelter, Harvey said.
Hospitals that shelter in place might limit admissions to emergencies. A lot goes into making those decisions, including deciding if the hospital has enough food, water, medication and backup generators for power.
Since Hurricane Katrina in 2005, hospitals have had to be self-sufficient on generators for seven days. Only three days of self-sufficient power were required before Hurricane Katrina, according to Harvey.

Evacuating a nursing home or assisted-living facility also is quite an ordeal and requires lots of preparation and planning, according to Kristen Knapp, director of communications at Florida Health Care Association, which represents nursing homes and assisted-living facilities in the state.
"It takes from 24 to 36 hours to evacuate a nursing home that has about 120 residents," Knapp said. "During Dorian, we had 19 nursing homes that evacuated and about 87 assisted-living facilities."
To add to the stress, hurricanes can be unpredictable. Dorian's wrath wasn't as bad as predicted in Florida as the storm hugged the coastline.
But that's not always the case. "It was really challenging during Hurricane Irma (in 2017) because that storm looked like it was going to hit the East Coast [of Florida] and at the last minute it shifted and hit the West Coast," Knapp said. "We had buildings that evacuated from the East Coast over to the West Coast and then very quickly they had to evacuate again."
"Evacuation is just a very stressful experience on nursing home residents," she said. "Certainly, they have to go with all their medications (and) if they use oxygen. Nurses accompany them. If you can shelter in place, that's an ideal situation, but sometimes you can't."
Responding to storms in Florida is a team effort, according to Knapp. Sometimes, it's nurses who come to the rescue of other nurses. The power was out for several days after Hurricane Michael hit Florida's Panhandle last year.
Nurses in the area were working long hours and needed relief not only from their jobs, but also to tend to their personal lives. Since Florida is part of the Nurse Licensure Compact, nurses with multi-state licenses could work in the state to provide the much-needed relief, Knapp said.
Nurses are pivotal during disasters, according to Harvey. Acute-care nurses usually can pitch in anywhere they're needed in a hospital -- from the emergency department to the pharmacy -- and they're patient advocates, which is critically important during a disaster.
"Nurses are very good at assessing situations and coming up with ways to handle them," she said.
With each storm comes lessons in how to best respond. Some employers, for example, have learned from the worst storms that it's best to have nurses' families and pets shelter in hospitals while nurses are on duty. That, according to Harvey, helps nurses do their jobs without worrying about their families and pets.












