In a Facebook poll, we asked nurses, how many steps they log per nursing shift?Your answers were astounding. With all the walking you do, the right nursing shoes can soothe those steps.
One nurse said she logged between 4,000 and 8,000 steps on a weekend shift -- around two to four miles, and many others logged a solid 8,000 steps per shift. Other nurses who shared their step counts logged thousands more steps, averaging between 10,000 and 12,000 steps. A few of you even logged as many as 20,000 steps during a 12-hour shift! Joint, back and foot pain may seem like an expected part of the job, given the amount of time nurses spend on their feet. But experts who specialize in foot care urge you to reconsider this assumption.
Educating nurses about optimum foot care
Kate Clayton-Jones, MSN, MBA, RN, CFCS, CFCN, was working as a nurse at a Massachusetts hospital when she started specializing in the foot care field in graduate school. "I noticed an incredible number of nurses complaining about their feet hurting at the end of their shifts," Clayton-Jones said. 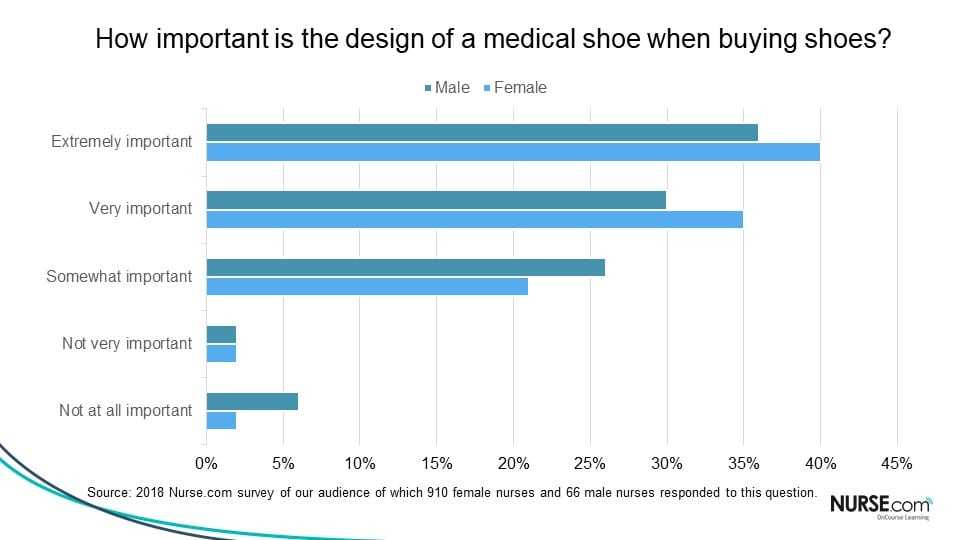 She began informally educating nurses about how their feet, legs, and muscles worked together, and she offered suggestions about how to select shoes that could reduce or eliminate pain.
She began informally educating nurses about how their feet, legs, and muscles worked together, and she offered suggestions about how to select shoes that could reduce or eliminate pain.
According to our recent survey, 75% of female respondents and 67% of male respondents said the design of a medical show was either very important or extremely important when buying shoes.
When asked about comfort, 88% of female respondents and 83% of male respondents reported comfort was extremely important when buying medical shoes.
Tips on nursing shoes and foot comfort

There are some simple ways to maximize comfort for nurses who may be walking up to 50 miles a week on the job. We talked to Clayton-Jones, founder of FootCare by Nurses, about best practices for selecting nursing shoes.
Q: What is the first step in picking the right nursing shoes?
A: Many people think their shoe sizes remain the same over time, but weight gain and swelling can change the width and volume of our feet. This can add as much as an additional shoe size. It's important to use the foot measuring device in a store to get a rough idea of the right sizing for your shoes. If you measure a size 8, you may need anywhere between a 7.5 to a 9 depending on the shoe.
Q: What types of shoes will maximize comfort?
A: Start by looking for shoes that fit the activities you'll be doing on your shift. I recommend shoes with a heavier sole that can absorb the impact of concrete, such as a good walking or hiking shoe. But nurses should avoid soles that are too stiff, like clogs, because the foot is supposed to flex to allow blood and lymph to circulate.
Q: How do I find a nursing shoe that matches my foot?
A: I encourage nurses to trace the general outline of their feet on a piece of paper and cut it out before they go to the store. This serves as their unique foot pattern. This is important because every foot is different. Some people may have long toes, a short foot and a narrow heel while others may have short toes, a long foot and a wide heel. Both will measure the same shoe size, and shoes are made in a variety of shapes. Try removing the insert and comparing it to your cut out or foot. It should match. People sometimes believe that spending more money on a shoe will maximize comfort, but no amount of money will create comfort if the shoe pattern doesn't match your foot pattern.
Q: Are there any other ways to avoid foot pain?
A: Once you've found nursing shoes that are designed for the work load and fit your feet, the next important step is properly securing the shoe to your foot. This can be done with lacing or a correctly positioned strap. The heel should be secured in the heel of the shoe. Otherwise, the foot may slip forward, which can either cramp the toes or force them to hold the shoe onto the foot. Gripping the toes can increase the risk of plantar fasciitis, hammertoe and other injuries.
Q: When should nurses start focusing on foot care?
A: I usually treat patients who are older, and I've seen what happens to the back, legs, and joints when people spend 20 to 30 years in a career without taking care of their feet. If instructors start teaching nursing students about the importance of foot care, they will enter the profession knowing that their feet and legs should not hurt. They also can be role models and teachers for others who follow their lead. The reality is that nurses are hard workers. If they apply a little bit of nursing knowledge to their feet, they will feel better and even have enough energy to go on a walk after a full day of work.
Tips for taking care of your toes
Liberated toes are critical for maintaining good balance and relieving tension. Follow these tips to improve balance and keep toes, feet, and legs healthy:
- Be mindful of where you are putting your weight on your feet. Physics changes the shape of our feet.
- Weight should mainly be on the heels and outside foot, not on the inside, forefoot or toes.
- Practice tension and release with your feet pointing in different directions.
- Encourage blood flow into the toes by wiggling them often.
- Massage and loosen the toes after work.
- Use lotion, creams, and oils that are gentle to the skin, such as olive or coconut oil.
If you wear nursing shoes that are comfortable and take care of your feet, they will support you and ease your pain.












