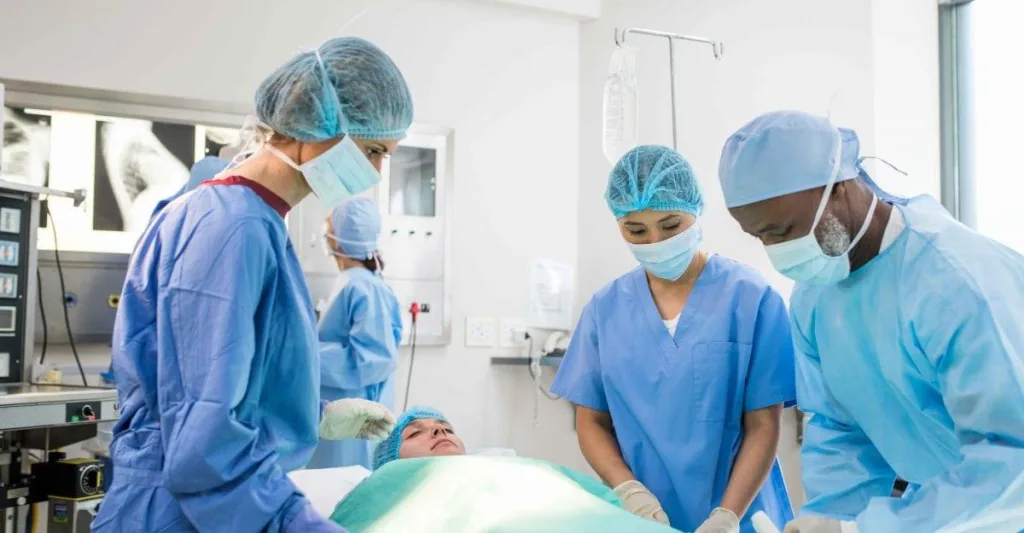
When nurse recruiters at Greenwich Hospital in Connecticut were struggling to fill OR nurse positions in 2016, Reynaldo De La Cruz, RN, CNOR, suggested starting a new residency program.
The program would allow nurses with no perioperative experience to learn the skills needed to work in the specialized operating room environment. For years, the hospital had been unable to compete with salaries for seasoned OR nurses offered in nearby Manhattan, New York. [caption id="" align="alignright" width="169"] Reynaldo De La Cruz, RN[/caption]
Reynaldo De La Cruz, RN[/caption]
"We often had great, experienced candidates and offered them positions, but when they heard the salary, they would back out," said De La Cruz , an OR nursing education specialist at Greenwich Hospital.
In an era when fewer nursing school programs or hospitals offer OR training, the residency would allow potential OR nurses a much-needed opportunity to learn. The interest in the program was clear when 50 nurses applied for six positions. As the program's creator, De La Cruz was careful to select nurses who were both talented and passionate about working in the OR because the participants who completed the residency would be offered full-time positions in the hospital's surgery department.
OR nurse shortage is regional phenomenon
Like Greenwich Hospital, facilities throughout the country are struggling to fill OR nurse positions as more RNs reach retirement age. According to a survey of more than 3,700 perioperative nurses conducted by the Association of periOperative Registered Nurses (AORN) in 2018, 73% reported the OR nurse shortage has had a moderate-to-crisis effect on their working environment. A total of 34% reported retirements were one of the reasons for the shortage, according to the survey.
[caption id="attachment_55108" align="alignright" width="214"]
Linda Groah, RN[/caption]
The demand for OR nurses also has increased in recent years as more surgeries are performed in the outpatient setting, said Linda Groah, MSN, RN, CNOR, NEA-BC, FAAN, CEO and executive director of AORN.
The number of ambulatory surgery centers grew from 3,000 to more than 5,600 in the last three years, she said.
The OR nurse shortage is projected to be most acute in the same states that are experiencing the general nursing shortage, Groah said.
The states include:
- California
- Texas
- New Jersey
- South Carolina
As facilities grapple with vacancies for OR nurse positions, an increasing number of hospitals have started developing nurse residencies, but these programs require funding, hospital space and instructors, Groah said. At Greenwich Hospital, De La Cruz successfully advocated for funding and he agreed to teach the residents. The first cohort, which included medical-surgical nurses and a cardiac telemetry nurse, learned about topics such as the principles of sterility, sutures, anesthesia and how to prepare for cases. In addition to classroom lectures, the 12-month program included clinical rotations with preceptors from different surgical specialties, such as general surgery, gynecology, urology, orthopedics and ear, nose and throat. The students also spent time in all three phases of surgery: preoperative, intraoperative and postoperative. Elizabeth Vitale, RN, one of the participants in the first cohort, had worked in a cardiac telemetry unit when she started searching for opportunities to learn OR nursing skills.
"The residency program was definitely a challenging experience, but it prepared us to work in the OR," said Vitale, who recently completed the program and now works in the hospital's OR. "I love the fast-paced teamwork environment."
The program was so successful that De La Cruz is planning to offer it again in September 2019 to help the hospital meet the demand for OR nurses in its outpatient surgery center.
The value of hospital space
Nurse leaders at RWJBarnabas Health in New Jersey foresaw the potential for a shortage of perioperative nurses in the future, which prompted the organization to launch an OR nurse training program in 1999. Yet one of the program's ongoing challenges was finding rooms to teach participants. [caption id="attachment_55110" align="alignright" width="200"] Mary Koch, RN-BC[/caption] "We had to plan classes around the availability of space," said Mary Koch, MSN, RN-BC, CNOR, director for the Center for Professional Development, Innovation and Research and coordinator of perioperative education at RWJBarnabas Health. When the system's Rahway Hospital closed a labor-and-delivery unit that was formerly an operating room area, leaders of the OR nurse training program suggested transforming the unit into a teaching space. "The unit had two operating rooms and would give the students the ability to practice repeatedly in a simulation environment," said Mary Beth Russell, PhD, MA, RN-BC, NEA-BC, vice president of the Center for Professional Development Innovation and Research Northern Region at RWJBarnabas Health. On Jan. 30, the simulation center opened with new manikins that will allow students to practice skills like inserting a catheter, assessing lung sounds and drawing blood. [caption id="attachment_55112" align="alignleft" width="216"]
Mary Koch, RN-BC[/caption] "We had to plan classes around the availability of space," said Mary Koch, MSN, RN-BC, CNOR, director for the Center for Professional Development, Innovation and Research and coordinator of perioperative education at RWJBarnabas Health. When the system's Rahway Hospital closed a labor-and-delivery unit that was formerly an operating room area, leaders of the OR nurse training program suggested transforming the unit into a teaching space. "The unit had two operating rooms and would give the students the ability to practice repeatedly in a simulation environment," said Mary Beth Russell, PhD, MA, RN-BC, NEA-BC, vice president of the Center for Professional Development Innovation and Research Northern Region at RWJBarnabas Health. On Jan. 30, the simulation center opened with new manikins that will allow students to practice skills like inserting a catheter, assessing lung sounds and drawing blood. [caption id="attachment_55112" align="alignleft" width="216"] Mary Beth Russell, RN-BC[/caption] About 60 students graduate from the program each year, and Koch predicts more students will be accepted now that there is space for a consistent rotation in a simulation lab. Tiffany Kamal, BSN, RN, had been working as a catheter lab nurse when she started considering the possibility of working in the operating room. She searched online for training opportunities in the area, and the program at RWJBarnabas Health was the only one she could find. She started the program in September 2017 and is now working in the operating room. "I really enjoy the team atmosphere where we are all empowered to speak up," Kamal said.
Mary Beth Russell, RN-BC[/caption] About 60 students graduate from the program each year, and Koch predicts more students will be accepted now that there is space for a consistent rotation in a simulation lab. Tiffany Kamal, BSN, RN, had been working as a catheter lab nurse when she started considering the possibility of working in the operating room. She searched online for training opportunities in the area, and the program at RWJBarnabas Health was the only one she could find. She started the program in September 2017 and is now working in the operating room. "I really enjoy the team atmosphere where we are all empowered to speak up," Kamal said.
How to attract new graduates to OR nursing
Like RWJBarnabas Health, University of Texas MD Anderson Cancer Center in Houston offers a perioperative nurse residency program, but leaders of the program were interested in drawing more new graduates to the training opportunity. "As we started to have more jobs available in the OR and many new graduates looking for jobs, we became more open to the idea of hiring new graduates," said Ri Dorado, MSN, RN, CNOR, director of perioperative nursing at MD Anderson. In the past, hiring managers had been hesitant to recruit new graduates because of the complexity of the cases at the specialized cancer center. To introduce more students to the perioperative specialty, the hospital recently started offering a two-week training to senior nursing students enrolled at the University of Texas Medical Branch in Galveston. The first three students, who participated in December 2018, learned through lectures and shadowing a nurse in the operating room at MD Anderson. While attracting talented nurses to work in the operating room is valuable, Dorado also recognized retaining nurses in the OR residency program was equally critical. Based on feedback from trainees, he started incorporating nurse managers into the orientation program, so they could provide feedback and support for the participants.
Although strategies like these are somewhat new, Dorado already has seen an increase in retention rates for new operating room nurses. And he's always open to opportunities that could eventually lead to new hires.
"Even if a surgical tech wants to observe a procedure, I make that possible," Dorado said. "We need to show other departments that we are not a scary unit."
Take these courses related to OR nursing:
Apply Perioperative Evidence-Based Practices to Put Sacred Cows Out to Pasture (1 contact hr) As with other specialties, gone are the days that perioperative nurses do things because, "This is the way we have always done it." When a practice or action is commonplace, the perioperative nurse should ask two questions: "Why are we carrying out this practice?" and "Is there sufficient evidence to support this action?" If you can't answer them, it's time to formulate a question and start an investigation to determine if evidence exists to support the questioned practice. This continuing educational module will challenge some "sacred cows" and provide guidance to help evaluate available studies so you can put them out to pasture. RNs Lead the Way in Managing Surgical Patients' Skin Integrity (1 contact hr) Pressure injury affects the more than 2.5 million hospitalized patients each year in the U.S. Studies have shown that patients who develop pressure ulcers have an increased rate of mortality. The people most affected are older adults and people with a major injury or comorbid disease. In the OR, management of a patient's skin integrity is a challenge. Anesthetized patients cannot adjust their position in response to physiological discomfort and lack of sensation. The state of anesthesia (general, local, block, or sedation) and anesthetic agents may compromise physiological response to ischemic tissue under pressure. Pressure injury may not be noticed until up to four days postop, and it may appear as a reddish-maroon or purple area by floor personnel. In the OR, the injured area may look reddish, which is caused by reperfusion after prolonged ischemia. This module will provide nurses with evidence-based practice changes that will promote their management of skin integrity in the OR. Anesthesia in the Perioperative Setting (1 contact hr) In 2010, 48.3 million surgical and nonsurgical procedures performed as ambulatory surgery. Patients consider anesthesia to be a major risk of surgery and expect perioperative team members to be their advocates by caring for their pre- and intraop needs and providing safe and effective care. This continuing education module discusses medications and anesthetics used in the clinical setting; anesthesia-related problems, such as aspiration, injection of bolus anesthetic agents, and malignant hyperthermia; and the nurse's role in dealing with these problems.
Prepare for the CNOR exam with the Operating Room Nurse Certification Review Course.
Nurse.com offers a fully online self-paced prep course.